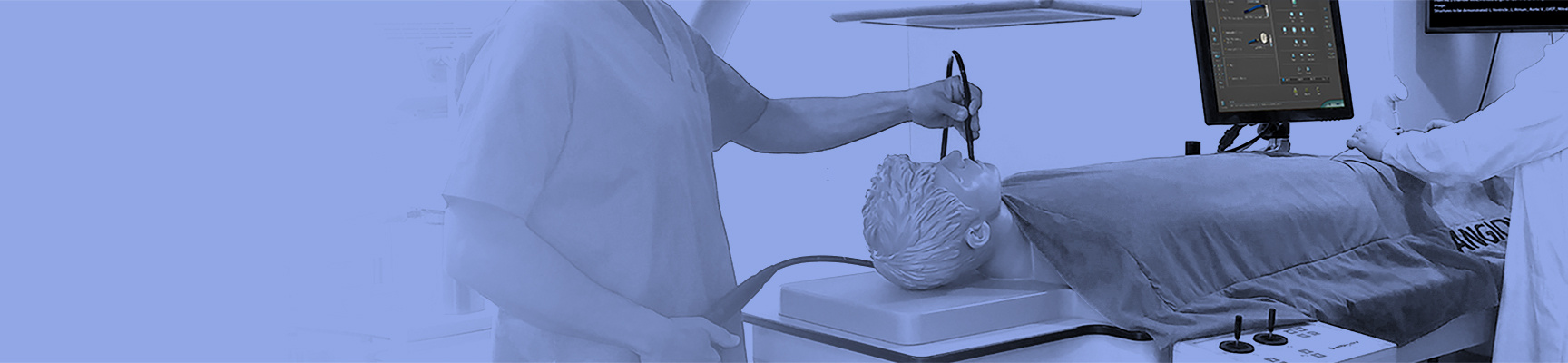
Unparalleled Endovascular Interventions Training

The ANGIO Mentor simulator is an essential tool for clinicians to practice and acquire the skills needed for performing endovascular interventions. Trusted by medical associations, hospitals, training centers, and the medical device industry globally, it provides trainees with realistic clinical settings to practice endovascular interventions using fluoroscopic and ultrasound guidance.
With a library of over 35 modules, growing with the evolution of endovascular techniques and devices, the simulator caters to 11+ medical specialties and offers training from basic skills to advanced interventions.
How To Improve a Physician’s Competency
See how ANGIO Mentor plays a prominent role in Dutch vascular surgeons certification.

Features and Benefits
-
Offers true-to-life simulation of the clinical environment, including advanced imaging modalities like fluoroscopy/echocardiography, hemodynamic monitoring, medications, and interventional devices
- Available in various platforms to fit any need, from stationary, human-sized manikin to ultra-portable platforms
-
Proven as a highly validated and effective simulator, with 30+ studies showcasing its effectiveness
-
Enables patient-specific simulation and custom case creation, tailored to your training needs
-
Simulates rare and common intra-procedure complications, allowing for realistic training in a safe environment
-
Comes with MentorLearn – our powerful and learning management system, enabling detailed performance feedback, customization of curricula and benchmarks
Modules
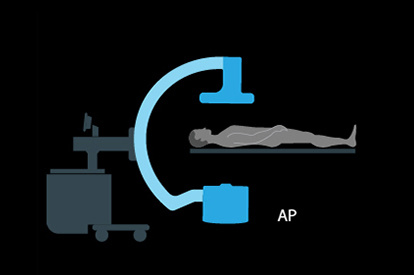
C-arm Basic Skills Module
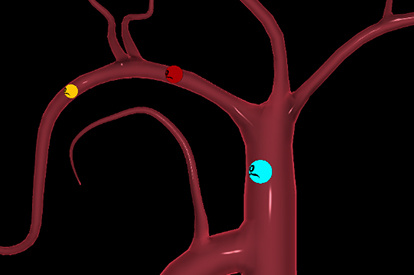
Endovascular Basic Skills Module
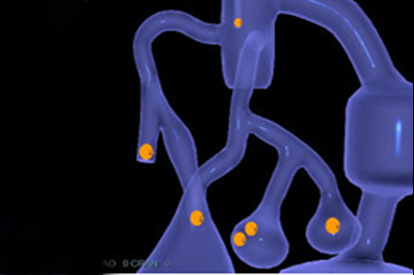
EP Basic Skills Module
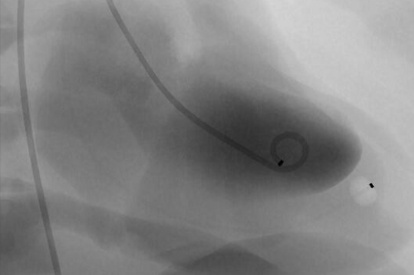
Cardio Basic Skills Module
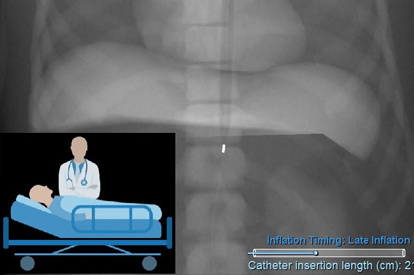
Bedside Cardiac ICU Module
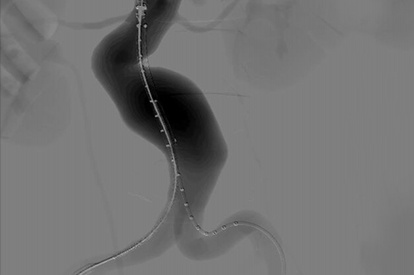
EVAR (Endovascular Aneurysm Repair) Module

TEVAR Module
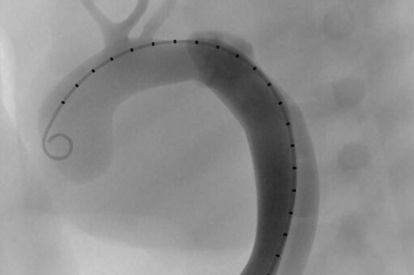
Advanced TEVAR Module
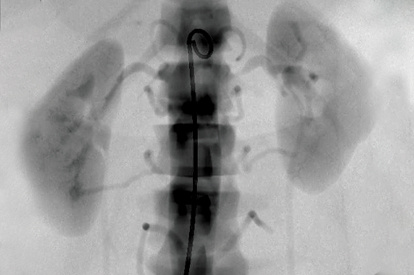
Renal Intervention Module
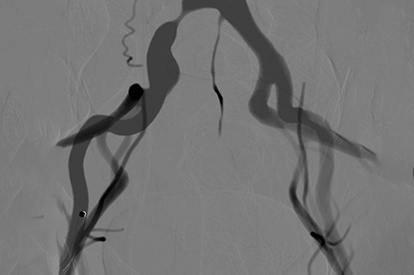
Iliac Intervention Module
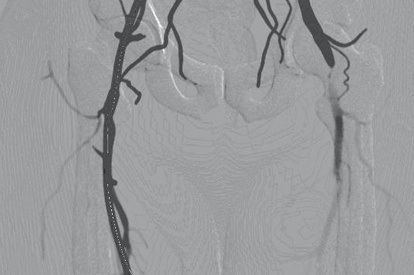
SFA Intervention Module
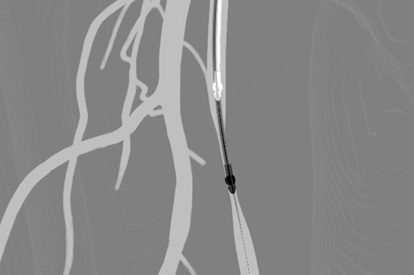
Atherectomy Module
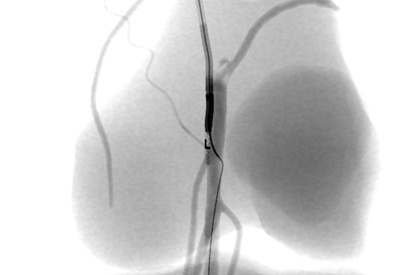
Lower Extremities CTO Module
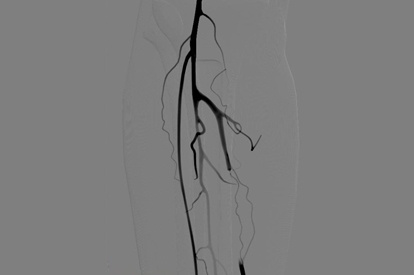
Below The Knee Module
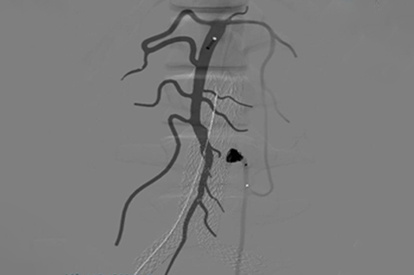
Peripheral Embolization Module
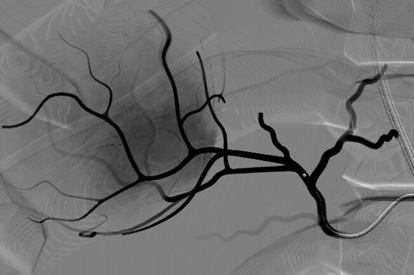
Embolotherapy (HCC & UFE) Module
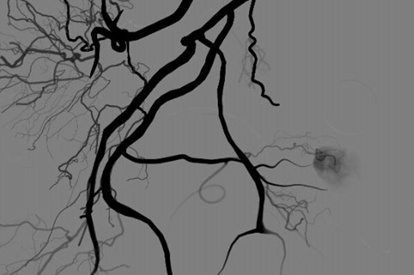
Prostatic Artery Embolization Module
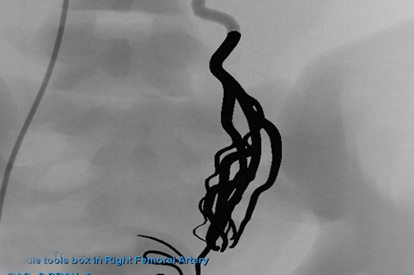
Advanced Embolization Module
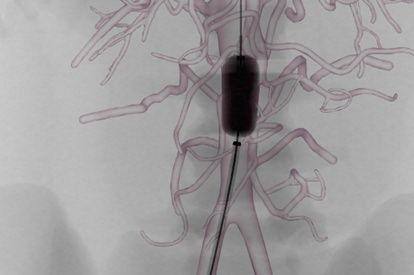
Endovascular Trauma Management Module
Venous Intervention Module
Carotid Intervention Module
Cerebral Intervention Module
Transradial Cerebral Module
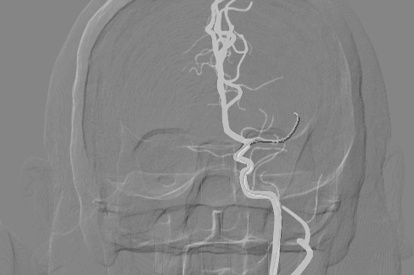
Acute Ischemic Stroke Module
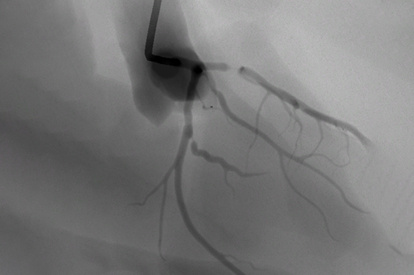
Coronary Intervention Module
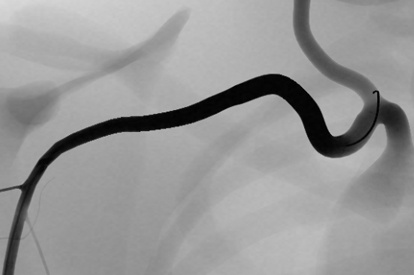
Transradial Coronary Intervention Module
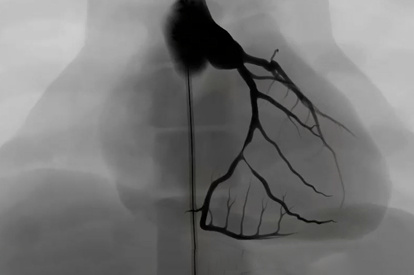
Coronary Bifurcation Module
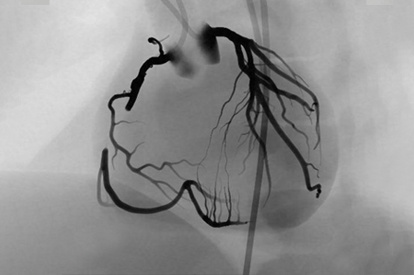
Coronary CTO Module
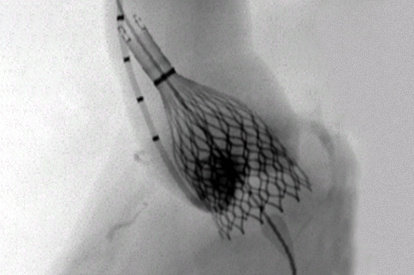
TAVI (Transcatheter Aortic Valve Implantation) Module
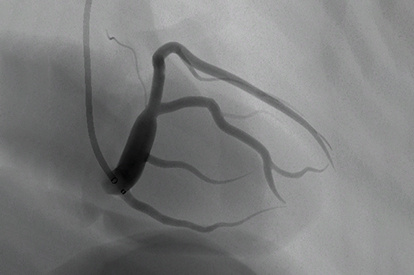
Cardiac Rhythm Management (CRM) Module
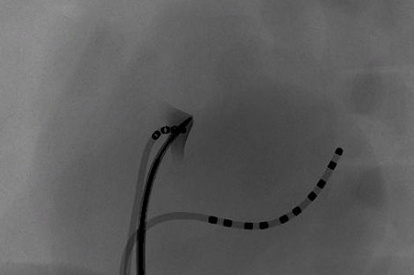
Transseptal Puncture Module
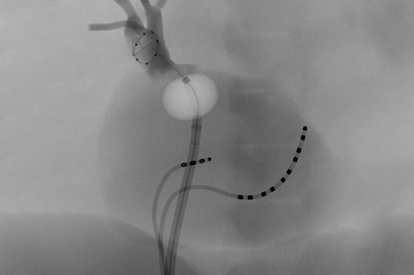
AF Ablation Module
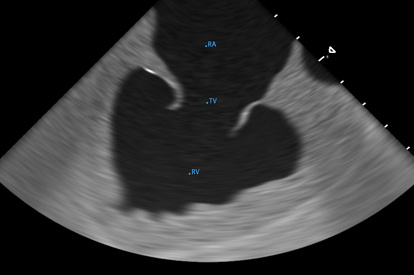
ICE Trainer Module
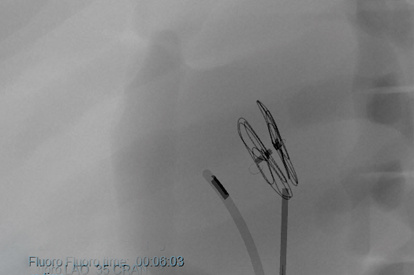
ASD-PFO Closure Module
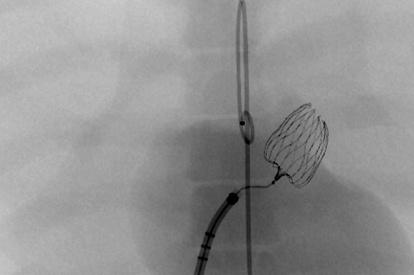
LAA Closure Module
EP Mapping Module
Testimonials
“What I like about the simulator is although you have the possibility to trigger complications in the middle of a procedure, the simulator will also react to any mistakes the trainee does. I particularly…
Prof. Iris Grunwald
Diagnostic and Interventional Neuroradiologist and Clinical Professor for Imaging and Science and Technology at University of Dundee, Scotland
"I believe that training on a Simbionix ANGIO Mentor should become an integral part of any endovascular curriculum. It provides residents and fellows with step-by-step training on fundamental skills…
Prof. Jean Bismuth
Associate Professor and leading vascular surgeon. Methodist DeBakey Heart and Vascular Center, Methodist Hospital, Houston, Texas
"Simulation training provides the opportunity to train demanding, new operations in a zero-risk environment for the patient. Our vascular surgery residents simply do not come close to patients until…
Dr. Jonash Eiberg
Department of Vascular Surgery and Copenhagen Academy of Medical Education and Simulation at Rigshospitalet and University of Copenhagen, Denmark
Simulators will have a place in the future to plan a procedure. They are not only for training. They allow us to look at the anatomy and try devices before we actually start the procedure
Horst Sievert MD, PhD
Director of the Cardiovascular Center and department of Internal Medicine, Sankt Katharinen, Frankfurt Germany.
“Historically one might say that I’ve been a “simulator skeptic.” But, I was utterly amazed with what Simbionix has accomplished: a thoroughly impressive recreation of complex aneurysm coiling… I have…
Dr. Thomas Masaryk
Chair, Neuroradiology Department, Cleveland Clinic
“I remember my days as a new intern….the first cases I performed were very difficult and it was a scary experience, since it takes between 10-20 procedures until you really feel that you are proficient.…
Prof. Michael Glikson
Director of Electrophysiology and Pacing at the Sheba Medical Center, Israel
“One of the outcomes of this nationwide course we are doing for 9 years is that the level of (endo)vascular knowledge and skills (competencies) in all regions in the Netherlands is clearly improved…
Prof. Bob Geelkerken
Consultant vascular surgeon, University of Twente, former chair of Dutch Society of Vascular Surgery
"We must train physicians that are currently performing old practices, on new devices and techniques. In addition, we needed a tool to train our residents and fellows without risking our patient. Now…
Dr. Nabil Chakfe
Vascular Surgeon, Head of GEPROVAS, and Head of the Department of Vascular Surgery and Renal Transplantation at Strasbourg University Hospital
“We use the Simbionix ANGIO Mentor for all our trainings because it gives us the opportunity to discuss best practices for TAVI, the device, different scenarios, complications management and it is used…
Violaine Carlier
Heart Valves Marketing Manager, UK & Ireland
“We have been using the ANGIO Mentor for training of our Gore Flow Reversal System. Our goal is to train physicians on procedural steps to maximize the effectiveness of the Gore Flow Reversal System…
Silvia Talco
Neurovascular European Product Manager WL GORE & Associates Srl.
“After extensive experience with another product and thorough research of all available options, we purchased an ANGIO Mentor in 2006 for our research and educational program. The ANGIO Mentor has lived…
Karl A. Illig
MD, Professor of Surgery and Neurosurgery, Chief, Division of Vascular Surgery, University of Rochester Medical Center
Validation Studies
Overall, ANGIO Mentor was the most highly validated and effective simulator and was the only simulator to achieve an LoE of 5/5.
Trainees who completed PROSPECT showed superior technical performance in real life with significantly fewer supervisor takeovers compared with trainees receiving e-learning alone. A structured, stepwise, proficiency-based endovascular curriculum including e-learning and simulation-based training should be integrated early into training programs to enhance trainee performance.
Download the ANGIO Mentor Brochure
Learn more about the ANGIO Mentor simulator.
Contact Us
Do you want to know more about the ANGIO Mentor?